What are Varicose Veins?
When we think of varicose veins, we may think of the big bulging veins that appear on the arms or legs. In reality, varicose veins have many more characteristics than just being visible on the skin. Varicose veins describe a condition in which the veins stop working properly, fill up with blood, and enlarge or swell due to a high volume of fluid build-up. Patients who experience varicose veins often complain of leg pain, a heavy feeling in their legs, numb or cold legs, leg cramps, and the appearance of blue or red bulging veins. While some patients may find relief from their varicose veins by wearing compression socks or stockings, many patients find they need to turn to medical attention. The specialists at StrideCare are more than happy to figure out which treatment options may be best for you during your one-on-one consultation.
What are Varicose Veins?
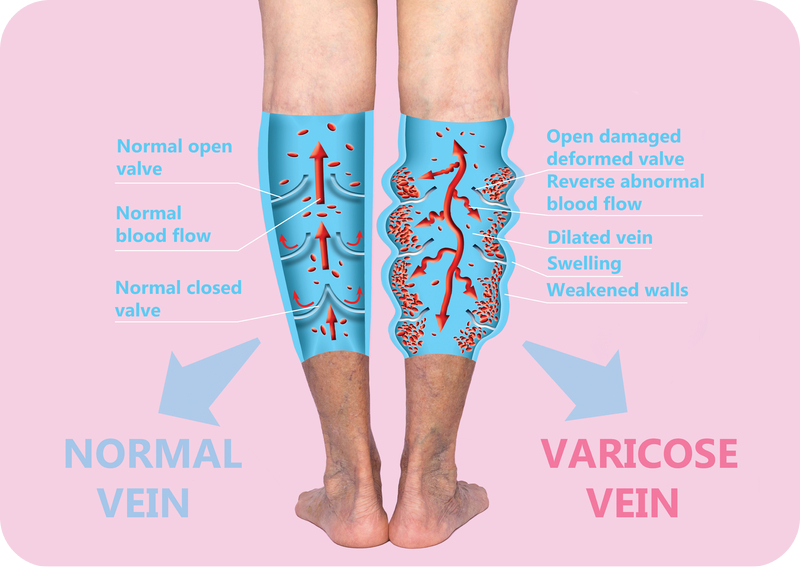
What Causes Varicose Veins?
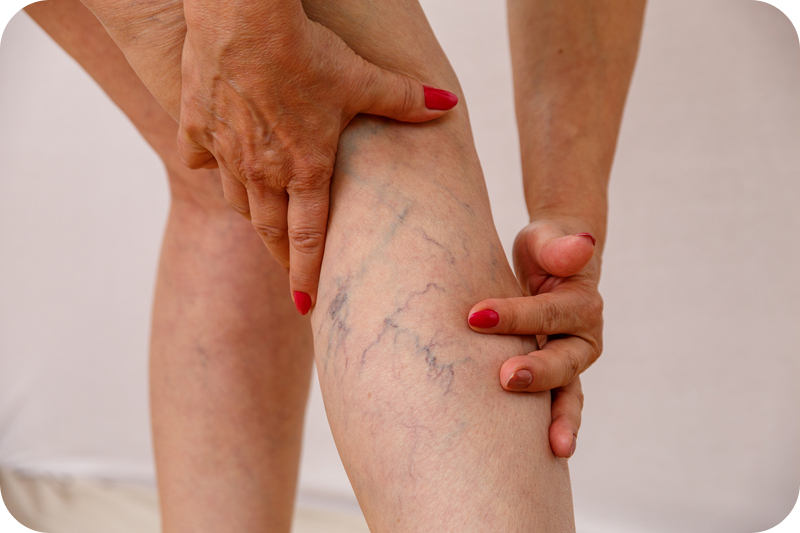
What Causes Varicose Veins?
Varicose veins appear when the veins in your body stop functioning properly. Typically, veins work on a one-way system using valves to keep the blood from flowing back in the wrong direction. When these valves fail, the veins pool with blood and cause a bulging appearance, skin discoloration, and discomfort. While varicose veins typically affect older patients whose bodies are naturally going through changes, other patients may also experience varicose veins if they are pregnant, are in their first stages of menopause, are obese, or have a family history of vein disorders.
What are the Symptoms of Varicose Veins?

Achy or heavy legs

Burning

Cramping leg

Lower leg swelling
Itching and tingling

Pain
What Treatments are Available for Varicose Veins?
There are Many Treatments for Varicose Veins Available at StrideCare Including:

Diagnostic Venous Ultrasound
Radiofrequency Ablation
Uses a small catheter to emit radiofrequency waves into the affected veins, which cuts off blood flow and relieves symptoms caused by varicose veins.
Varithena™ Microfoam Ablation
Treats both varicose and spider veins using a concentrated, injectable foam.
Spider Veins, Varicose Veins, Reticular Veins:
What’s the Difference?
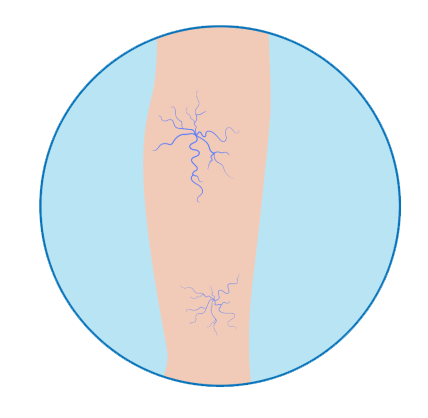
Spider Veins
- Measures about 1-1.5mm
- Pink, red, or purple
- May be painful
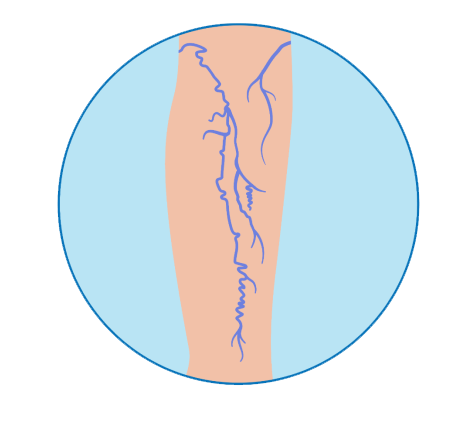
Reticular Veins
- Measures about 2mm
- Color varies from green-blue to purple
- Can burn and/or itch
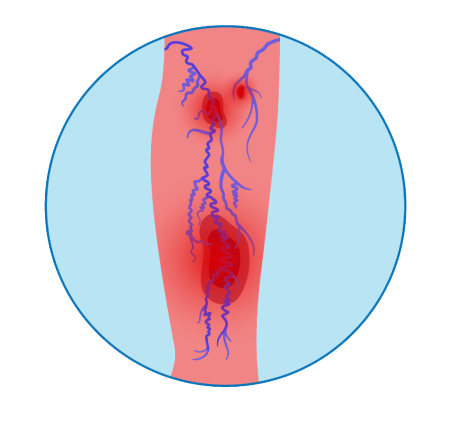
Varicose Veins
- 2.5mm or larger
- Dark blue or purple color
- Often protrude above the surface of the skin and can lead to pain, burning, and spasms
StrideCare
Patient Reviews



4.89 Average Online Review Score












StrideCare Leverages athenaOne to Enhance Financial and Operational Results, Improve Clinical Workflows
2 Min Read CASE STUDY: Transitioning all practices onto one united system gives StrideCare invaluable access to data
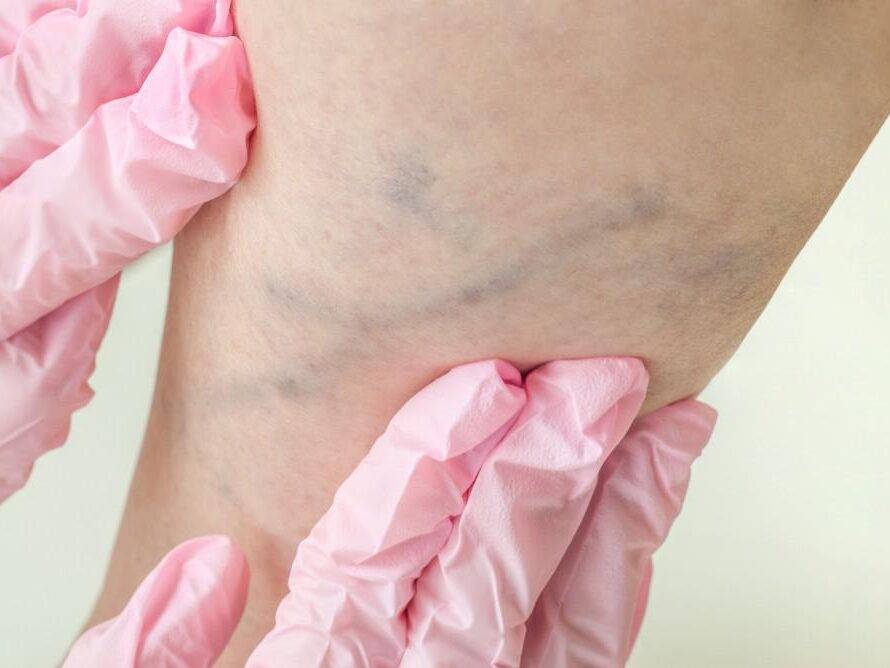
When are Varicose Veins More than Just a Cosmetic Concern?
2 Min Read Learn about varicose veins, prevention tips, and treatment options from StrideCare’s vein specialists in Texas.
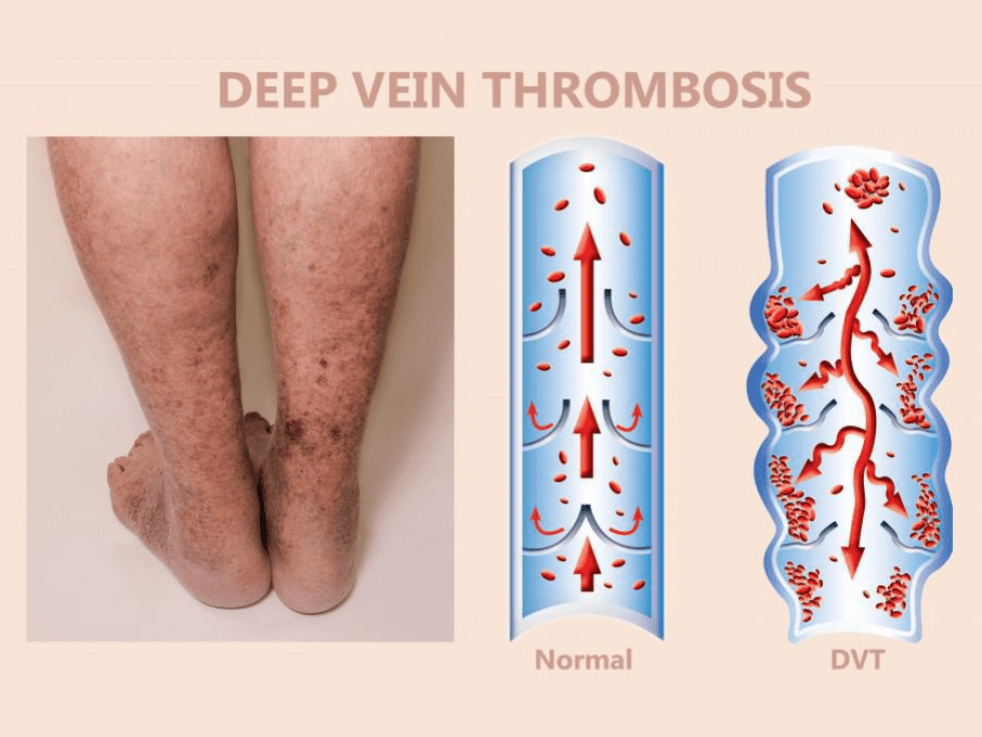
Puffy Legs are One of the First Signs of Deep Vein Thrombosis
3 Min Read Learn the symptoms of deep vein thrombosis (DVT) and seek immediate evaluation at StrideCare for expert care and treatment.


